BONES, FRACTURES AND DISLOCATIONS
What bones are made of
To understand why bones break, it helps to know what bones do and what they are made of. The bones of the body form the human frame, or skeleton, which supports and protects the softer parts of the body. Bones are living tissue. They grow rapidly during one’s early years and renew themselves when they are broken. Bones have a center called the marrow, which is softer than the outer part of the bone. Bone marrow has cells that develop into red blood cells (which carry oxygen to all parts of the body) and white blood cells (which help fight disease). Bones also contain the minerals calcium and phosphorus. These minerals are combined in a crystal like or latticework structure. Because of their unique structure, bones can bear large amounts of weight.
How fractures occur
People often think that a fracture is less severe than a broken bone, but fractures are, in fact, the same as broken bones. Bones are rigid, but they do bend or “give” somewhat when an outside force is applied to them. When this force stops, bones return to their original shape. For example, if you fall forward and land on your outstretched hand, there is an impact on the bones and connective tissue of your wrist as you hit the ground. The bones of the hand, wrist and arm can usually absorb this shock by bending slightly and then returning to their original shape and position. If the force is too great, however, bones will break, just as a plastic ruler breaks after being bent too far.
People often think that a fracture is less severe than a broken bone, but fractures are, in fact, the same as broken bones. Bones are rigid, but they do bend or “give” somewhat when an outside force is applied to them. When this force stops, bones return to their original shape. For example, if you fall forward and land on your outstretched hand, there is an impact on the bones and connective tissue of your wrist as you hit the ground. The bones of the hand, wrist and arm can usually absorb this shock by bending slightly and then returning to their original shape and position. If the force is too great, however, bones will break, just as a plastic ruler breaks after being bent too far.
Types of fractures
The severity of a fracture usually depends on the force that caused the fracture and the strength of the bone. If the bone is bent only slightly, then the bone may crack rather than breaking all the way through. If the force is extreme, such as in an automobile collision or a gunshot, the bone may shatter. If the bone breaks in such a way that bone fragments stick out through the skin or a wound penetrates down to the broken bone, the fracture is called an “open” fracture. This type of fracture is particularly serious because once the skin is broken, infection in both the wound and the bone can occur. “Closed” fractures — breaks in the bone that do not cause it to stick through the skin — are the more common type of fracture. All fractures are either open or closed.
Signs/symptoms of a fracture
Signs that a fracture has occurred include: being unable to move the affected area, complaints of pain with movement, deformity, and swelling. The medical team will examine you to determine if any of these signs are present. They also will check to see if you have movement, sensation, and circulation to the area below the possible fracture.
Dislocations
A dislocation occurs when a joint exceeds its range of motion so that the bone is no longer in its socket. When dislocations occur, there may be a large amount of soft tissue injury in the joint capsule and surrounding ligaments and muscle, with possible vein, artery, and nerve damage. Signs of dislocations include: severe pain, joint deformity, inability to move the joint and swelling. The team may attempt to relocate the limb (called a reduction) while in the ED or the operating room.
Risks and complications of a fracture and/or dislocation
The following are other injuries and potential complications that may occur when a bone has fractured or become dislocated. Blood vessel injury: Patients who fracture a bone also may have injuries to the veins and arteries surrounding the broken bone. These types of injuries can cause bleeding or loss of blood flow below the injured area. The team will follow your bleeding studies, examine the injured limb, and check your pulses and circulation closely. Sometimes further studies - like an angiogram - and / or surgery may be required to repair the damaged vein or artery.
Compartment syndrome:
Patients with severe fractures or crush injuries are at risk for developing compartment syndrome — a condition that occurs most frequently in the leg or forearm. Compartment syndrome causes increased pressure in the soft tissues that, in turn, causes decreased blood supply to the affected muscles and nerves. This decreased blood supply can lead to damage if the pressures are not relieved. The team will check you closely for signs of compartment syndrome, which include: throbbing pain that does not become better with pain medicine; swelling and increased pain to the muscle when it is stretched; and firmness over the compartment. Doctors have a device to check pressures in the compartment when this syndrome is suspected. If compartment pressures are high, you will be taken to surgery for a procedure called a fasciotomy. In this procedure, the compartments are opened up to relieve the pressure. Once swelling to the area goes down, the team will close and cover these wounds.
Damage to nerves:
Patients with fractures may also experience damage to the nerves close to the injured area. To diagnose potential nerve injuries, the team will ask you if you can move and/or feel the affected limb. Some nerve injuries may improve with time as swelling around the area decreases.
Deep Vein Thrombosis (DVT): A DVT is a blood clot that develops in one of the blood vessels in the leg or pelvis. Trauma patients are at risk for developing DVTs because of both the nature of the injury and the inactivity associated with it. Trauma patients often need to stay in bed for a period of time until their injuries are stabilized or repaired. Signs of DVT include pain or tenderness over the injury site, swelling, fevers and/or changes in skin color. The team will order a special radiological test that looks for blood clots in your body and may take precautionary measures such as giving you blood thinning medicine and devices to wear on your legs called “pneumo boots” to prevent DVTs from forming.
Infection: All fractures put you at increased risk for infection. However, open fractures (fractures in which the skin is broken) put patients at even higher risk for infection. Wound and bone infections can be disabling for patients because they can delay or prevent healing of the fracture. Open fractures are evaluated in the ED, where patients are given antibiotics and a tetanus vaccine. If you have an open fracture, you will be taken to surgery right away, so that the fracture site may be cleaned. If the wound is not completely clean, it will be kept open to the air, while the fracture will be immobilized with a cast, splint, traction, or an external fixator. You will return for more surgery in about 48 hours to see if the wound needs cleaning. If it is clean at this time, the wound may be closed and internal fixation may be performed. There are times when the wound may be too big to close. When this occurs, a skin graft or local muscle flap will be placed to cover the wound.
Pneumonia: A patient who cannot or does not get out of bed frequently may develop pneumonia — a result of fluids building up in the lungs. Signs of pneumonia include fever, chills and a cough. The team may order an x-ray of your chest to detect pneumonia and may give you an antibiotic to treat it if diagnosed. You can help prevent pneumonia by coughing and breathing deeply on a regular basis and by getting out of bed as soon as the team feels it is safe for you to do so.
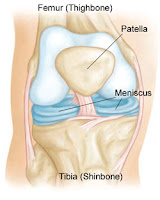
Post-traumatic arthritis: Fractures that involve the joint have a higher risk of developing arthritis (inflammation of the joint) at some point after healing has taken place. Early treatment of these fractures and proper healing reduce this risk.
Pulmonary embolism (PE): A pulmonary embolism — commonly referred to as a “PE” — is a blood clot that develops in the leg or pelvis and then travels through the bloodstream to the lungs, where it can cause problems. A trauma patient who is not active is at risk for developing a PE. Signs of this type of complication include shortness of breath, difficulty breathing and taking short and rapid breaths. A patient who is suspected to have a PE will be given oxygen and placed on a monitor to evaluate heart rate and how much oxygen is entering the bloodstream. He/she will also undergo a special test that searches for this type of clot.
Pulmonary embolism (PE): A pulmonary embolism — commonly referred to as a “PE” — is a blood clot that develops in the leg or pelvis and then travels through the bloodstream to the lungs, where it can cause problems. A trauma patient who is not active is at risk for developing a PE. Signs of this type of complication include shortness of breath, difficulty breathing and taking short and rapid breaths. A patient who is suspected to have a PE will be given oxygen and placed on a monitor to evaluate heart rate and how much oxygen is entering the bloodstream. He/she will also undergo a special test that searches for this type of clot.
Swelling and blisters: Injury to the soft tissues near the fracture or dislocation site can occur, resulting in bruising and swelling to the area. The swelling can be significant and possibly cause blisters. You may be instructed to keep the affected limb elevated and/or apply ice to help decrease the swelling. The team will
examine the fractured area to watch for the development of blisters. Significant swelling and blister formation can cause surgery to be delayed.
Prepared by BWH
examine the fractured area to watch for the development of blisters. Significant swelling and blister formation can cause surgery to be delayed.
Prepared by BWH


Dr marcos tive 3 fraturas numa perna do joelho pra baixo,foi colocado uma haste do joelho ate o tornozelo ,beleza mais agora doe do lado da perna da umas fisgada nos ossos ,queria saber se é normal pq o osso ta colando nao sei bem,
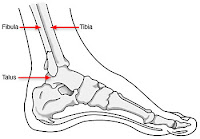
ResponderExcluirA fratura da tíbia frequentemente esta acompanhada da fratura da fíbula que é um osso lateral na perna, essa fratura em geral é fixada indiretamente com a haste intramedular da tíbia porém pode doer um pouco enquanto cicatriza. Converse com seu ortopedista.
Excluir